Millions of people live with one or more missing teeth, and the effects go far beyond appearances. Missing teeth can change how you chew, alter speech patterns, and gradually affect the underlying jawbone and facial structure. Modern implant dentistry addresses these concerns by restoring function and form in a way that closely mirrors natural teeth.
Dental implants are titanium posts placed in the jaw that act as artificial tooth roots. Once they integrate with bone, implants provide a stable foundation for crowns, bridges, or full-arch restorations. Because they restore both the root and the visible portion of a tooth, implants deliver more predictable long-term outcomes than many tooth-replacement alternatives.
At M. Kurt Berky, DDS, PC, we focus on patient-centered implant care that balances predictable surgical technique with esthetic prosthetic results. Whether you need to replace a single tooth or rebuild an entire arch, implants allow us to design solutions that preserve oral health while restoring confidence and comfort.

The key advantage of implants is how they interact with the jaw. By integrating directly with bone, an implant provides the kind of support that mimics a natural tooth root. This direct support translates into biting strength, stability while speaking, and a secure foundation for a life-like crown or denture.
Because the prosthetic tooth attaches to an anchored implant instead of relying on neighboring teeth, there is often less alteration of healthy tooth structure. That means adjacent teeth can be preserved rather than being drilled or crowned to support a bridge. For many patients, this conservative approach contributes to better long-term oral health.
Implants also help maintain the jawbone. When a tooth is lost and not replaced by an implant, the bone that once supported it can shrink over time. Implants provide functional stimulation to the bone, helping to preserve the natural contours of the face and the integrity of the underlying structure.
Successful implant treatment starts with careful assessment. We evaluate bone quantity and quality, soft tissue health, occlusion (how your teeth come together), and overall medical factors that influence healing. Clear planning helps determine whether a single implant, several implants, or a full-arch solution is the best path forward.
Once a treatment plan is established, implant placement is performed using techniques and technology that prioritize precision. Many approaches include guided or computer-assisted planning to position implants in the optimal location for function and esthetics. This attention to detail reduces complications and supports a smooth restorative phase.
After the implant is placed, the body gradually bonds to the implant surface in a process called osseointegration. Once integrated, the implant supports a custom-made crown, bridge, or denture designed to blend with your smile and restore chewing ability. With proper care and maintenance, implants are a highly reliable method for tooth replacement.
Implants differ from conventional bridges and removable dentures in several important ways. They recreate both root and crown, which often leads to improved stability, comfort, and function. For many patients this means fewer dietary limitations and less worry about slippage or adhesive use.
Because implants don’t rely on neighboring teeth for support, healthy adjacent teeth often remain untouched. This preserves natural tooth structure and can reduce the need for additional restorative work in the future. Patients also frequently report a more natural feel when speaking and eating compared to removable prostheses.
Long-term maintenance of implants centers on the same basics as natural teeth: good home care and professional checkups. With regular hygiene and periodic evaluations, implants offer a durable and dependable solution for replacing missing teeth while supporting overall oral health.
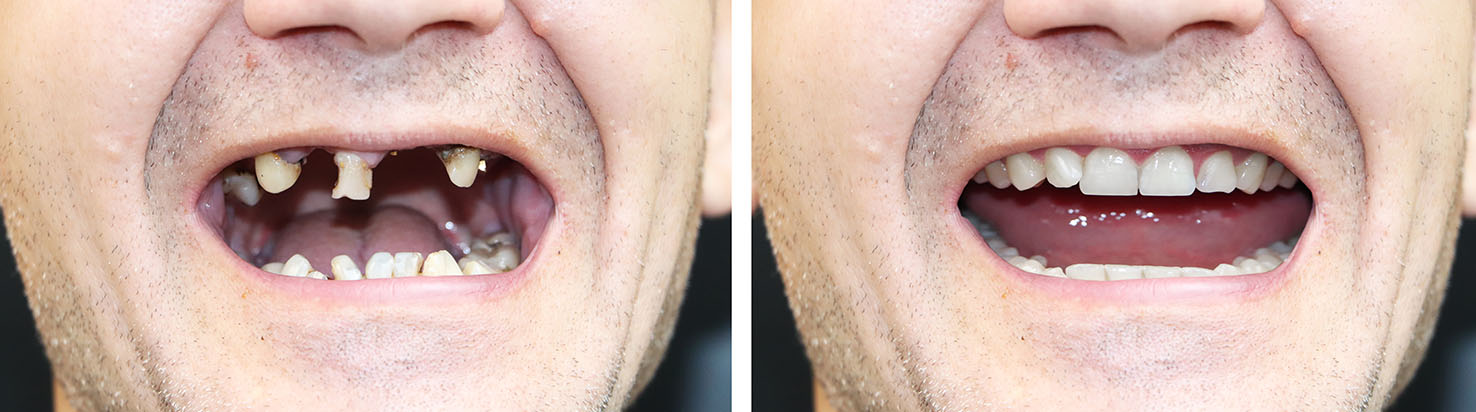
A single implant capped with a carefully matched crown can replace an individual missing tooth with minimal impact on adjacent teeth. This option restores chewing function and esthetics while leaving neighboring teeth intact, which is often preferable to methods that require altering healthy teeth.
Because the implant stands on its own, the resulting crown can be designed precisely to match size, shape, and color, creating a seamless appearance in the smile line. For patients who value conservative treatment, a single implant is a strong choice.
When several teeth in a row are missing, implant-supported bridges use strategically placed implants to anchor multiple replacement teeth. This approach restores chewing function across a span without burdening adjacent healthy teeth, and it provides the bone stimulation necessary to maintain the supporting jaw.
These restorations are engineered for durability and esthetics, and they come in a range of materials and designs to meet patient needs. Because the structure is supported by implants rather than natural teeth, long-term wear patterns tend to be more favorable.
For patients missing an entire upper or lower arch, full-arch implant strategies can provide life-changing improvements. Fixed full-arch restorations attach permanently to a set of implants, restoring a stable, non-removable replacement that functions much like natural teeth.
Alternatively, implant-retained overdentures connect to a smaller number of implants with attachments that allow removal for cleaning while significantly improving retention and comfort compared with conventional dentures. Both approaches eliminate many of the limitations associated with older denture designs.
Candidacy for implants depends on a combination of oral and systemic factors, including bone volume, gum health, general medical history, and personal goals for treatment. Many patients who once thought they were not candidates are able to proceed after targeted bone or tissue procedures that prepare the site for reliable implant placement.
We evaluate each case individually and discuss options that align with your oral health, cosmetic expectations, and lifestyle. Our goal is to develop a treatment plan that balances predictability with the look and feel you want from your restored smile.
If you’re curious about implants but unsure whether they are right for you, our team will explain the options and the steps involved so you can make an informed decision with confidence.
Good outcomes begin with careful planning. Advanced imaging and careful measurements guide implant positioning so the prosthetic teeth will be both functional and esthetic. Planning also helps us anticipate whether bone grafting or soft-tissue enhancement is needed before or during implant placement.
When planning is complete, we review anesthesia and comfort measures so you understand how the procedure will be performed and what to expect during recovery. Clear communication and preparation are central to a smooth surgical experience.
Implant placement is typically performed on an outpatient basis and can range from a straightforward single-placement to a more complex site-preparation procedure. Most patients tolerate the surgery well, and downtime is usually brief. After placement, a period of healing is required for the implant to integrate with the bone before the final restoration is attached.
In some cases, temporary restorations can be delivered immediately for improved function and appearance during healing. Our team will explain which approach makes the most sense for your situation so you know what to expect at each step.
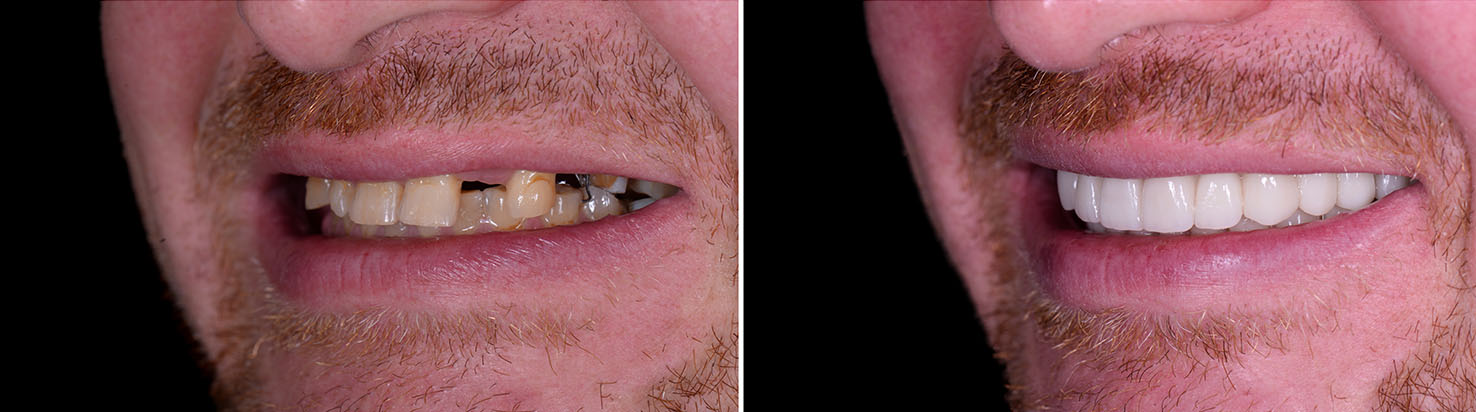
Sufficient bone volume is essential for a stable implant. If bone has been lost due to prior extractions, periodontal disease, or trauma, a graft can rebuild the foundation needed for predictable implant support. Bone grafting is a routine procedure and can be performed before, during, or after implant placement depending on the individual case.
Grafting restores the support necessary for long-term success and makes it possible for many patients to receive implants who otherwise might not be candidates. We discuss grafting options and the expected healing timeline as part of a comprehensive treatment plan.
Replacing missing teeth is about more than filling a gap — it’s about restoring function, preserving oral health, and rebuilding confidence. With a focus on thoughtful planning and precise execution, implant dentistry offers a durable and natural-feeling solution for many patients.
At M. Kurt Berky, DDS, PC, our team combines restorative skill with careful surgical planning to help patients reclaim healthy, attractive smiles. If you would like to learn more about implant options or discuss a personalized treatment plan, please contact us for more information.

If you've lost a tooth due to injury, decay, gum disease, or any other reason, we recommend dental implants to replace missing teeth. Dental implants come the closest to replicating the look, feel, and function of your natural teeth.
Dental implants are placed into the jawbone and mirror the same function as the root of a tooth. The procedure for dental implants is usually performed while a patient is sedated. Patients who undergo IV sedation must have an empty stomach and transportation home following the procedure. Most sedation patients will have little to no memory of the procedure occurring.
Generally, dental implants are made out of a biocompatible metal such as titanium. Biocompatible metals are also used for other common bone implants (such as shoulder, hip, and knee replacements). The visible portion of the implant is usually made out of porcelain and is custom-made to match your existing teeth.
Dental implants are designed to fuse to the bone, which makes them become permanent fixtures. Typically speaking, the success rate is nearly 100%. There are few cases in which the implant will not fuse as intended and must be removed. If this happens to occur, the procedure can be attempted again a few months later.
Dental implants are not usually covered by dental insurance, but may be covered under a patient's medical insurance. Our office and your insurance company can discuss coverage options with you based on your individual case and treatment plan.
It's easy... just take care of an implant as if it's a natural tooth! This involves regular brushing, flossing, and dental checkups. If you have any concerns about your implant, contact us immediately.
Dental implants are small, biocompatible posts that are surgically placed into the jawbone to replace the root of a missing tooth. After placement, the implant integrates with the surrounding bone tissue through a process called osseointegration, which creates a stable foundation for a crown, bridge, or denture. The visible restoration is attached to the implant and is designed to match the appearance and function of a natural tooth.
Implants restore chewing function and help preserve jawbone volume by stimulating the bone where a natural tooth root once existed. Because they act like natural tooth roots, implants reduce the likelihood of shifting teeth and can help maintain facial contours. Proper planning and imaging are used to determine the optimal size, position, and type of implant for each patient.
Good candidates for dental implants are generally adults in overall good health with sufficient jawbone to support an implant or the willingness to undergo preparatory procedures such as bone grafting. A thorough evaluation will consider your medical history, oral health, gum condition, and any habits that affect healing, such as smoking. Chronic conditions like uncontrolled diabetes or certain medications can influence candidacy, so candid discussions with your dentist and physician are important.
Bone quality and quantity are evaluated using clinical exams and 3-D imaging when needed, and minor procedures can often prepare a site for implant placement. Age alone is not a limiting factor; the primary considerations are healing capacity and oral health. Your dentist will present personalized options and recommend the best pathway to achieve a predictable result.
Implant restorations can range from a single crown to multi-tooth bridges and full-arch replacements. A single-tooth implant restored with a crown replaces one missing tooth without involving adjacent teeth, while implant-supported bridges use two or more implants to support multiple replacement teeth. For patients missing all teeth in an arch, full-arch fixed solutions or implant-retained dentures provide stable, functional replacements.
Implant-retained dentures attach to strategically placed implants for improved retention and comfort compared with conventional removable dentures. Fixed full-arch options can provide a permanent, non-removable restoration that closely resembles natural dentition in function and appearance. The appropriate restoration depends on the number of missing teeth, bone availability, and the patient’s functional and aesthetic goals.
The implant process begins with a comprehensive consultation and diagnostic planning, which may include digital X-rays or a cone beam CT scan to assess bone and anatomy. On the day of surgery, an implant post is placed into the jawbone under local anesthesia and, when appropriate, sedation to keep the patient comfortable. The surgical site is then allowed to heal while the implant integrates with the bone, a step that is critical for long-term stability.
Following osseointegration, an abutment is attached and impressions or digital scans are taken to design the final restoration, such as a crown or bridge. Temporary restorations may be used during healing when function and esthetics are a concern. Your dentist will provide specific pre- and post-operative instructions and schedule follow-up visits to monitor healing and progress.
Healing times vary depending on the implant site, bone quality, and whether any additional procedures, like bone grafting, were performed. Typically, the osseointegration period ranges from a few months to several months for complete bone integration before a permanent restoration is placed. Some treatment protocols allow for a temporary crown or provisional prosthesis immediately after placement, but the final restoration is scheduled once the implant is stable and the tissue has properly healed.
Your dentist will evaluate healing at follow-up appointments and will proceed with the final abutment and restoration when clinical and radiographic signs indicate successful integration. The goal is to ensure a durable and well-fitting restoration that supports proper function and long-term oral health. Individual timelines are discussed during the treatment planning phase so patients know what to expect.
Bone grafting is recommended when there is insufficient bone height or width to support a dental implant safely and predictably. Tooth loss, periodontal disease, infection, or long-term denture wear can lead to bone resorption, leaving a site that may not adequately anchor an implant. Grafting rebuilds lost volume and creates a more stable foundation for implant placement.
Bone grafts can use the patient’s own bone, donor bone, or synthetic materials, and the choice depends on the clinical situation and the amount of augmentation required. In some cases grafting is performed at the same time as implant placement, while in others it is completed as a separate procedure to allow for healing. Your dentist will explain why grafting may be necessary and outline the expected healing timeline and outcomes.
Long-term care for dental implants includes excellent daily oral hygiene, routine dental checkups, and professional cleanings. Brushing twice a day and interdental cleaning around implants using floss, interdental brushes, or water flossers helps prevent plaque buildup and maintains healthy gums and supporting bone. It is important to maintain regular dental visits to monitor implant health and to address any early signs of inflammation or complications.
Healthy lifestyle choices, including avoiding smoking and managing systemic health conditions, support implant longevity. Your dental team may recommend specific home-care tools and techniques for your restoration type and will provide individualized guidance on the frequency of professional maintenance visits. Prompt attention to any discomfort, swelling, or changes around an implant helps protect your investment and oral health.
While dental implants are a reliable tooth replacement option, potential complications can include infection, peri-implant inflammation, nerve or sinus-related issues, and implant failure in rare cases. Many of these risks are reduced through thorough planning, precise surgical technique, and careful patient selection. Proper oral hygiene and regular follow-up care are essential to minimize the chance of inflammatory problems around the implant.
Your dentist will review potential risks during the consultation and explain how they are managed, including antibiotic protocols, surgical precautions, and post-operative care instructions. Early detection and intervention are key to resolving most complications, and routine monitoring allows the dental team to act quickly if concerns arise. Clear communication about medical history and habits also helps customize care to reduce risk.
Modern implant care benefits from advanced imaging and digital workflows that enhance precision and predictability. Tools such as cone beam computed tomography (CBCT) and digital impressions improve diagnostic accuracy, treatment planning, and the fit of final restorations. Guided surgery techniques and computerized planning allow implants to be placed in optimal positions while protecting anatomical structures.
The practice also integrates restorative technologies that streamline fabrication of crowns and bridges and improve occlusal harmony. Sedation options and clear pre- and post-operative protocols support patient comfort during surgical procedures. The office of M. Kurt Berky, DDS, PC uses these proven technologies and techniques to help achieve reliable, esthetic implant results.
To schedule a consultation, contact the office by phone or the online appointment request to arrange an initial evaluation and imaging as needed. Bringing a list of current medications, relevant medical history, and any recent dental records or X-rays helps streamline the assessment. Photographs of your smile and notes about your goals and concerns are also useful for creating a personalized treatment plan.
During the consultation your dentist will perform a clinical exam, review imaging, discuss treatment options and timelines, and answer questions about the process and expected outcomes. If additional diagnostic imaging such as a CBCT scan is indicated, the office will arrange it so you and your dentist can make well-informed decisions about implant care. The practice is located at 29 Park Pl, Branford, CT, and staff can advise whether to call New Patients at (203) 309-1087 or Existing Patients at (203) 315-9909 to book your visit.

Have questions or need to book your next appointment?
Our friendly staff at M. Kurt Berky, DDS, PC is ready to assist. Whether by phone or our online contact form, contacting us is simple and convenient. Start your journey to a healthier, brighter smile today by reaching out to our office.